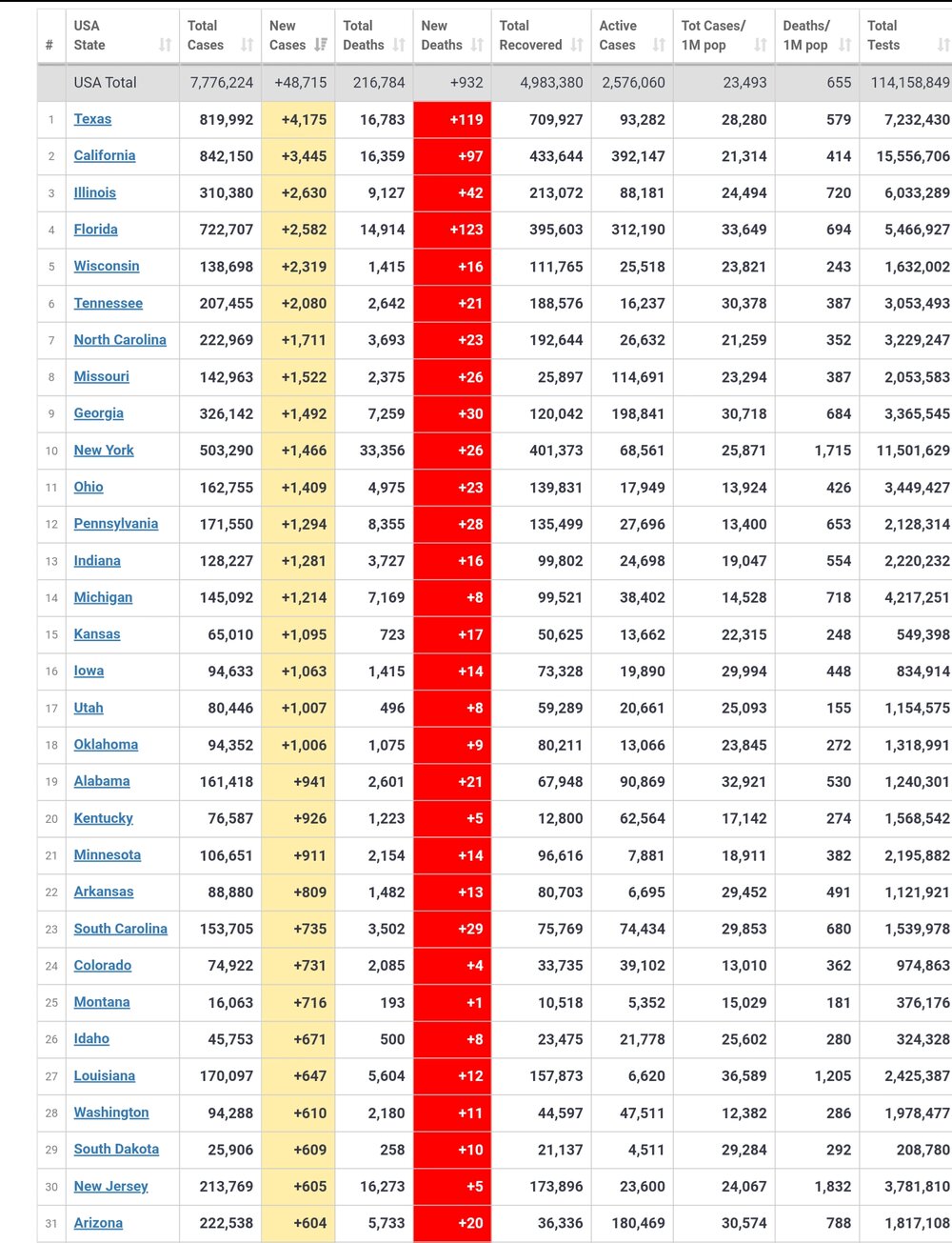
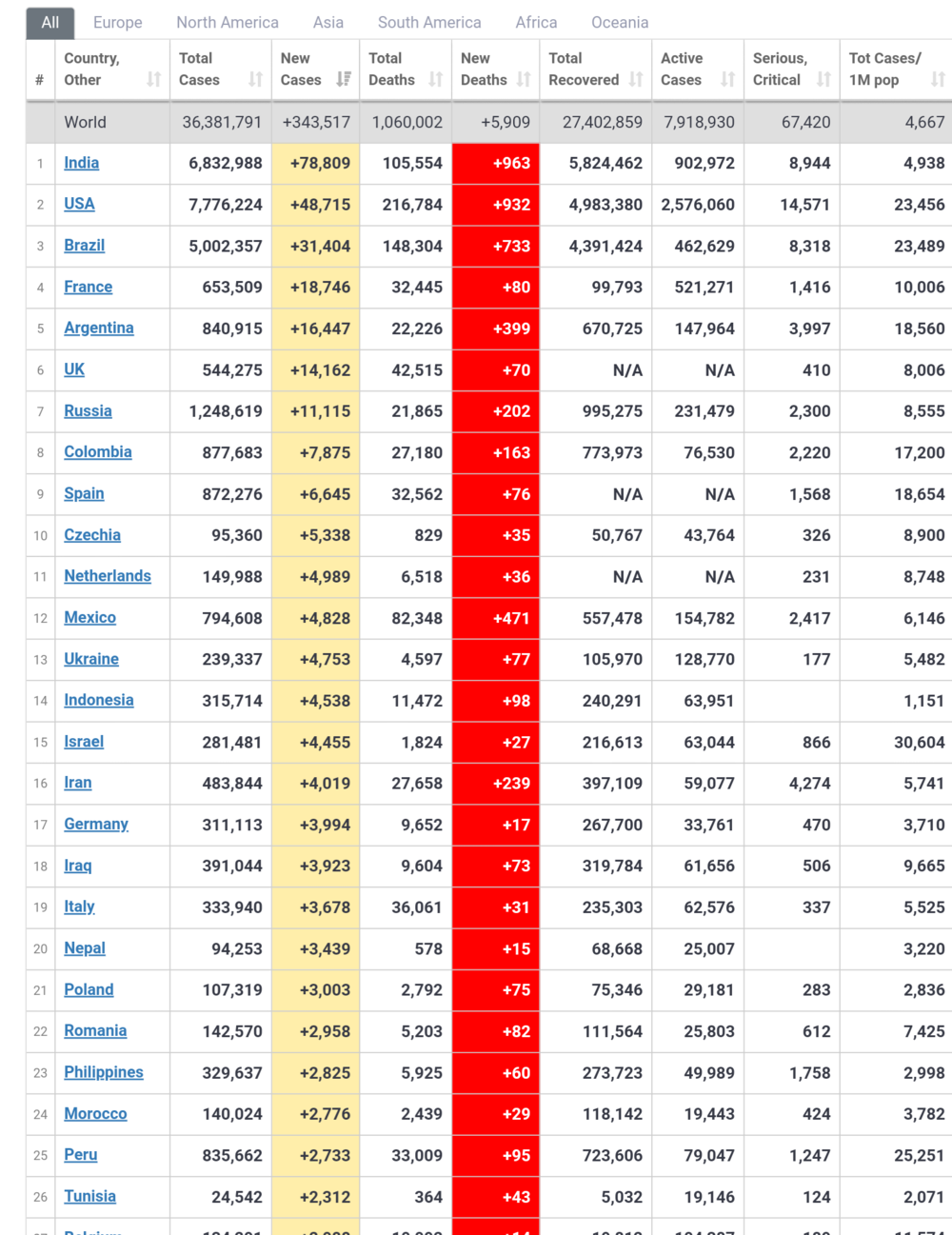
Researchers at Oxford's Centre for Evidence Based Medicine and the University of the West of England have published a pre-print of a scientific paper (i.e. one that has been submitted to a journal for peer review but has not yet been published) which is arguing the point that I have been making in this thread for some time: that a lot of new 'positive' cases are not infectious carriers of the virus, but rather people who got over the infection some time ago but are still shedding unviable viral fragments that are detectable with an RT-PCR test.
A press article about the study:
Coronavirus tests 'may be picking up traces of dead virus'
The preprint itself can be found here:
Viral cultures for COVID-19 infectivity assessment. Systematic review
The authors recommend more effort is made to distinguish between people who are testing positive for SARS-CoV-2 on RT-PCR tests, and those who are actually infectious, by more routine testing by viral culture growth from samples in supposedly infected individuals, better training of PCR testers and the establishment of a cut off in the cycle threshold of detectability in the PCR test in order to declare that someone is positive for the virus. They write
"An increasing body of evidence shows that such identification cannot be accurately achieved through the simplistic division of those who test positive and who do not on the basis of the results of RT-PCR [This is nevertheless how it is carried out in practice around the world - AD]
. The sensitivity and specificity of RT-PCR needs comparing to the gold standard of infectiousness: the capacity to grow live virus from a specimen.
[...]
"The purpose of viral testing is to assess the relation of the micro-organism and hazard to humans, i.e. its clinical impact on the individual providing the sample for primary care and the risk of transmission to others for public health. PCR on its own is unable to provide such answers.
[...]
"A binary Yes/No approach to the interpretation RT-PCR unvalidated against viral culture will result in false positives with segregation of large numbers of people who are no longer infectious and hence not a threat to public health."
They point out that viral shedding in the upper respiratory tract detectable by RT-PCR testing has been observed to occur up to 83 days after the onset of symptoms, but that the presence of viable virus, necessary for someone to be infectious to others, occurs only for a maximum of 8 days after the onset of symptoms.